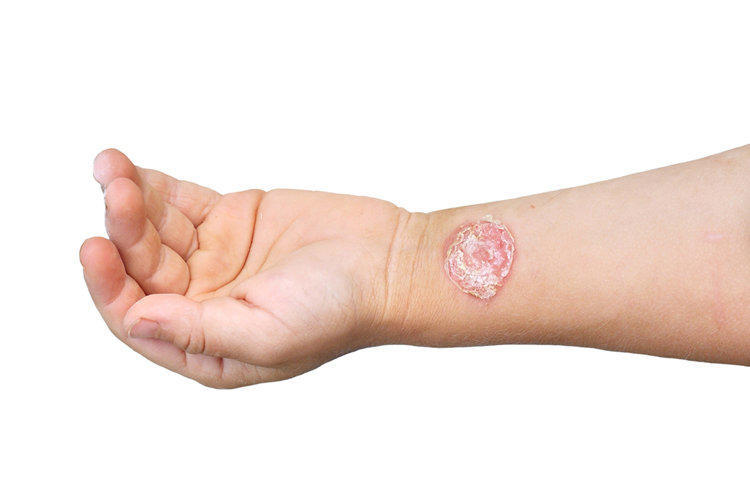
Streptoderma – a disease of the human skin of inflammatory etiology caused by streptococcus bacteria. Depending on the location and depth of penetration of pathogenic microflora into the skin layers, various types and types of streptoderma emit.
- Streptococcus: microorganism that causes streptoderma
- Skin injury as a factor in the development of streptoderma
- How Streptoderma Begins
- Causes of recurrence and complications in the treatment of streptoderma
- C treptoderma in children: forms and symptoms
- Streptococcal impetigo
- Slit-like impetigo
- nail felon
- Streptococcus diaper rash
- Dry form of streptoderma or Erimato-squamous
- Bullosa impetigo
- Actima vulgaris
- Streptoderma Diagnosis
- Streptoderma in children: types of treatment
- The Importance of Hygiene in Streptoderma Therapy
- Streptoderma : home treatment with antiseptic drugs
- Antibiotics for Streptoderma
- Systemic antibiotic therapy for streptoderma
- Streptoderma and similar diseases
- Pyoderma
- Herpetic eruptions
- Thrush or candidiasis
- Allergies
- Chickenpox
- Prevention of pyoderma caused by streptococcus
Children are most susceptible to the disease: streptoderma in children occurs more often than in adults due to the emerging skin immunity, an increased number of minor skin lesions and the inability to comply with all hygienic rules that prevent the onset of streptoderma. How to treat streptoderma in children depends on the age of the child and the characteristics of the clinical picture of the disease.
Streptococcus: microorganism that causes streptoderma
Streptococci are opportunistic bacteria present on the skin of each person. They are detected by analyzes of intestinal microflora, scrapings from mucous surfaces, samples from the inner surface of the respiratory tract. The size of microorganisms is so small that they can be seen only in photographs of streptococci created with multiple magnification through microscopes. However, the prevalence of bacteria and statistics suggest that everyone is familiar with streptococcal infection, and some people may be permanent hidden carriers that spread pathogens.
Streptococci are bacteria that survive well outside the human body: the period of viability lasts for months, and infection is possible when in contact with household items. During disinfection, these microorganisms die within 7-15 minutes, depending on the concentration of the solution, at a temperature of 60 ° C, neutralization begins after 15 minutes, at boiling points and above — instantly.
Streptococci are almost universal microorganisms that can cause not only streptoderma of different types, but also responsible for the development of scarlet fever, streptococcal angina , tonsillitis, pharyngitis, inflammation of the lungs of bacterial etiology, bronchitis, meningitis, myocarditis, glomeruli , erysipelas of the skin, lymphadenitis, promote the development of abscesses, etc.
Often, with streptoderma and abscesses, treatment is complicated by the addition of an additional microorganism – staphylococcus, also present on the skin and in the human body.
Skin injury as a factor in the development of streptoderma
Normally, streptococci live on the surface of the skin without causing harm to humans. Local skin immunity allows you to maintain a balance between beneficial and opportunistic microflora, not allowing microorganisms to destroy the layers of the epithelium. However, for the start of rapid reproduction and inflammatory process, it is enough for them to penetrate the layers of the skin through a scratch, crack, cut, comb of an insect bite. In this case, the injury of the epithelium may be microscopic and invisible to the eye. The phenomenon of streptoderma in the nose is one of the most frequent manifestations of streptoderma in children prone to studying the nasal passages with their fingers. Streptococci, inhabiting the skin or mucous membranes, are activated in the slightest scratches of mucous membranes left by children’s nails.
“Entry gates” for infection can also be damage to the skin that is not associated with mechanical trauma: manifestations of an allergic reaction, atopic dermatitis, urticaria, skin rash with chickenpox, etc.
How Streptoderma Begins
The causative agent of streptoderma may be present everywhere, and the likelihood of developing the disease largely depends on the immunity of the child and the number of pathogens on his skin or on contact with it.
Sources of streptococcal bacteria:
- the skin of the child himself, the carrier of streptococci;
- household items: dishes, furniture, toys, bedding, towels, etc.
- another child or adult, healthy carrier of bacteria;
- A patient with diseases caused by streptococci: streptoderma, tonsillitis, bronchitis, streptococcal pneumonia, and scarlet fever. In this case, the development of streptoderma is more likely, as contact occurs with aggressive bacteria that have multiplied under favorable conditions and require less time for activation.
Streptoderma in children’s institutions can occur as an epidemic outbreak, when a sick child is a source of infection and spreads pathogens. The latent incubation period for this disease ranges from 2 to 10 days.
How is the transmission of infection in streptoderma and other diseases caused by streptococci? An infection can be transmitted in the following ways:
- contact path: when touching, contacting the skin to the skin of a patient or carrier and a healthy person, when playing together children, kissing adults, etc.;
- household contact streptococcal infection occurs when using the same household items: dishes, toys, books, towels, etc.
- The most rare is the airborne mode of transmission when streptococcus moves from a sick person or carrier during coughing, sneezing to a damaged skin area.
Causes of recurrence and complications in the treatment of streptoderma
In some cases, streptoderma in children is prolonged. Treating streptoderma with relapses is difficult. This occurs in the absence of therapy, as well as in cases where the patient’s body cannot independently confront the pathogen due to the following reasons:
- the child has diseases that damage the skin: allergic, atopic dermatitis, pediculosis, scabies, or a tendency to combing bites, wounds, crusting, etc.;
- with a general decrease in immunity against the background of chronic or frequent diseases, anemia, helminth infections, inflammatory processes in the oral cavity with slit streptoderma (“stuck”), with prematurity, insufficient nutrition and other factors hindering the development of the immune system or reducing its protective functions ;
- streptoderma in the nasal passages, in the ears is difficult to cure in the presence of otitis media, rhinitis, accompanied by secretions, irritating mucous membranes and skin and promoting the growth of bacteria;
- under adverse living conditions: low hygiene, as well as exposure to low or high temperatures, which contribute to damage to the epidermis, sunburn, permanent or prolonged contact of the damaged surface with liquids, water (when bathing, occasional changing of the diaper, etc.);
- the accession of a secondary infection, staphylococcus, causes streptostaphyloderma, vulgar impetigo, which requires complex therapy directed against two pathogens.
C treptoderma in children: forms and symptoms
Depending on the form of the disease, streptoderma in children may cause temporary discomfort or be symptomatic. In severe forms, the following clinical picture of streptoderma is observed:
- The child’s body temperature rises to febrile indicators;
- symptoms of general intoxication of the body are observed: headache, muscle, joint pain, nausea, vomiting, lethargy, loss of appetite;
- local lymph nodes are enlarged, they can be painful on palpation;
- Blood tests show a characteristic picture of the inflammatory process.
The disease is normal with appropriate therapy takes from 3 days to two weeks, ending with recovery. Symptoms of streptoderma, the period of the acute stage depends on the form of streptoderma, localization of inflammation, its depth and severity, as well as the individual characteristics of the organism to resist infection.
Depending on the place of development of the inflammatory process, the depth of penetration of the pathogen into the skin and the severity of the disease, there are several forms of streptoderma. All of them belong to streptoderma, but have different names.
Streptococcal impetigo
Among all forms of streptoderma, this is the most common. It includes streptoderma that develops in the nasal passages, as well as small local skin lesions located on the face of the head, hands, feet and other open skin areas of the child.
This form of streptoderma is a superficial skin lesion, in which the initial development of the disease is opposed by the mechanism of local immunity, which limits the inflammatory process. It proceeds according to the following stages of the disease:
- on the outwardly tranquil part of the skin, flakten is formed – a dense bubble with a transparent or unclear contents up to 3 mm in diameter, redness occurs around;
- in the next stage, the bubble-conflict spontaneously opens or falls, a light yellow crust forms at the site of the lesion (drying out or weeping “sores” on the face);
- The crust separates, leaving patches of deep pink or pinkish-bluish color that disappear.
Each individual site of inflammation from onset to cure exists for 5-7 days. If therapy begins at the first stage of the appearance of a bubble, in most cases the infection affects the skin only once. However, if you do not pay attention to the manifestation of streptoderma, the pathogen spreads through the body during touching, bathing, toweling or sleeping, which causes multiple lesions. Such a disease can last from a month or more, causing a decrease in the overall immunity of the child and contributing to the spread of infection in the family and children’s groups.
Slit-like impetigo
This form of streptoderma is better known under the popular name “zaedy”: a narrow strip of inflamed skin in the form of a slit, which occurs most often in the corners of the lips, less often in the lateral folds of the eyelids, nose wings.
At the beginning of the disease, conflict is formed, as a rule – a single one. The disease in most cases is limited to one area of the skin, causing itching, soreness, discomfort, and resolves on its own or with minor local therapy.
However, with reduced immunity or the presence of inflammatory processes near the site of streptoderma (oral candidiasis, caries, gingivitis, conjunctivitis, rhinitis, etc.), the disease can turn into a chronic, sluggish stage, difficult to cure.
nail felon
Streptococcal inflammation of the skin around the nails develops when the pathogen enters the wound, most often with burrs or cuticle injury. Streptococcus can penetrate both from the surface of the skin around and when the injured area comes into contact with the environment or during the process of scratching the already existing streptodermia impetigo.
Felaria is expressed in redness, swelling, pain of the skin around the nail roll, the formation of cellulitis, erosive changes. Without treatment, it can lead to loss of the nail plate, spread of the pathogen through the bloodstream to other organs, and cause meningitis.
Streptococcus diaper rash
They usually appear in young children. Developed with the accession of streptococcal infection to skin lesions at the site of diaper rash, manifestations of dermatitis, allergies. The manifestation of this form of streptoderma with a high frequency is observed behind the auricles, in the inguinal skin folds, axillary folds.
Secondary lesion of damaged skin with streptococci leads to a merger of erosions, pain in the skin area, a long course, which is difficult to treat. The treatment is carried out during the treatment of the underlying disease.
Dry form of streptoderma or Erimato-squamous
Erimato-squamous streptoderma most often occurs on the face, sometimes on the limbs or trunk. Weeping elements characteristic of other types of streptoderma are absent, the disease is expressed in the appearance of patches of pink or reddish uneven rounded shape with a surface of exfoliating whitish epidermis.
This is one of the least active forms of streptoderma in distribution throughout the body, which does not cause any discomfort in the course of the flow. However, a high level of contagiousness requires both treatment and isolation of sick children.
Bullosa impetigo
This form differs in both appearance and more severe course of the disease. Most often, the hands, feet and legs, at the initial stage form large serous purulent bubbles, soft to the touch, with pronounced inflammation around. They tend to slow development. After spontaneous opening of purulent bubbles, places of open erosion are formed.
There may be a sharp deterioration in health, febrile temperature (from 38 ° C), an increase in local lymph nodes, signs of intoxication.
Actima vulgaris
Refers to the most severe forms of streptoderma. Streptococci infect the deep layers of the epidermis. The tissue is necrotized, ulcers are formed. The characteristic localization is the buttocks, lower limbs with possible exceptions.
Factors contributing to the development of vulgar ecthyma are a decrease in body resistance after SARS, influenza, chickenpox, measles, and intestinal infections, as well as hypovitaminosis, systemic diseases (diabetes mellitus of all types, diseases of the hematopoietic system, endocrinological pathologies).
It is difficult, requires complex therapy.
Streptoderma Diagnosis
Diagnostic measures for streptoderma may be limited to taking history and visual examination from a pediatrician or dermatologist. In some cases, to clarify the diagnosis, the presence of a primary disease and the composition of pathogenic microflora, additional examinations may be prescribed:
- laboratory analysis of blood parameters (general, biochemical);
- general urine test;
- feces analysis on helminth eggs;
- Sometimes they can prescribe a test for Wasserman reaction, the presence of immunodeficient states of viral etiology.
Streptoderma in children: types of treatment
All forms of streptoderma, even the lungs, must be accompanied by treatment, since the disease is highly contagious to others, without therapy, can affect large areas of skin and lead to severe complications.
The Importance of Hygiene in Streptoderma Therapy
Streptoderma is a disease in which the treatment of the hygienic factor plays an important role in the prevention of its development and in the spread of the pathogen to others. Treatment of streptoderma without hygiene may not have a therapeutic effect and lead to a protracted form of the disease.
Hygiene rules for all forms of streptoderma:
- Avoid wetting the affected area of skin, for 3-5 days, do not bathe the child, limiting yourself to washing separate parts of the body (legs, genitals) if there are no inflamed areas on them. Use wet wipes, towels, etc.;
- in the presence of pruritus, try to avoid scratching, touching the affected area, you can use antihistamines;
- use an individual towel, dishes for the patient, often wash and wash;
- all minor injuries and scratches on the skin are regularly treated with antiseptic preparations;
- To carry out regular hygienic cleaning of the room, to clean soft toys, bedding often wash and iron.
Streptoderma : home treatment with antiseptic drugs
For the local treatment of streptoderma in children at home, use antiseptic solutions and ointments. They need to wipe areas of inflammation. But in some cases it is necessary to carry out the opening of the bladder with the treatment of the affected area with an antibacterial agent. Only a medical professional should do this.
Treat streptoderma with the following antiseptics:
- hydrogen peroxide solution;
- fukortsin;
- salicylic alcohol;
- furatsilin;
- brilliant green (Zelenka).
Means are used to treat the affected area and the skin around it from 2 to 4 times a day. Zinc ointment can be used as a drying and disinfecting agent. To enhance the effect, it is possible to apply decoctions of camomile pharmaceutical , oak bark, flowers of the train.
Antibiotics for Streptoderma
Preparations of antibiotic groups are used in the treatment of the disease in forms that have local and systemic effects. How to treat streptoderma in children with antibacterial drugs, determines the specialist.
Medicines from the group of antibiotics used in streptoderma, can be either single-component, with one active ingredient, or combined. The combined drugs used in the treatment of various forms of streptoderma include local medicines (creams, ointments) with a combination of antibacterial and hormonal therapy.
| Antibacterial ointments and creams | Estimated cost, rub. | Combined Ointment | Estimated cost, rub. |
| Tetracycline | 60 | Lorinden | 290 |
| Erythromycin | 25 | Triderm | 680 |
| Lincomycin | 40 | Akriderm Ghent | 275 |
| Gentamicin | 40 | Akriderm | 300 |
| Sintomycin | 60 | ||
| Methyluracil | 60 |
Systemic antibiotic therapy for streptoderma
Penicillins are recognized as the group of first choice antibiotics in the treatment of various forms of streptoderma. In some cases, it is possible and appropriate to replace penicillin preparations with a cephalosporin group or macrolides.
When is penicillin not prescribed for streptoderma?
- if a child has an individual intolerance to the drugs of this group, allergic reactions to previously taken penicillins or allergens that cross to it;
- if in the near history there is a disease in the treatment of which penicillin-type antibiotics were used;
- If the resistance to microflora revealed high resistance of pathogenic microorganisms to penicillin.
Streptoderma and similar diseases
There are a number of diseases with manifestations on the skin, which at different stages of development may look like streptoderma. Most of the coincidences occur in the first stage of blistering, but there are similar to any stage of development of streptoderma diseases. It is for this reason that the specialist should carry out the diagnosis and choice of therapy.
Pyoderma
Pyoderma is a group of all purulent inflammations of the skin, and this group and all forms of streptodermia are included in this group. However, unlike other pyoderma, with streptoderma, the primary stage is more similar to the manifestation of a viral than a bacterial infection. Thus, other pyodermas of bacterial etiology differ from streptodermas by turbidity of the secreted and distinctive forms of the inflammatory process.
Herpetic eruptions
Manifestations of the activity of the human herpes virus on the lips are often confused with streptococcal zhedoy When differentiating, pay attention to three main differences:
- herpes rashes are localized on the intact area of the skin, all forms of streptoderma require skin injuries to develop;
- stages of development of streptoderma occur more quickly, bubbles fall or open within a much shorter period of time than with a herpes infection;
- with herpes, itching precedes the onset of rash, with streptoderma, itching occurs only when there is skin manifestation.
Thrush or candidiasis
Candidiasis of the oral cavity can spread to the corners of the lips and form cracks in the skin. Differentiation from pyoderma is carried out by the presence of characteristic white point lesions on the internal mucosa of the oral cavity, white plaque, ulcerated surface of the mucous under it.
Allergies
Some children may experience a nonclassical manifestation of a skin rash of an allergic etiology in the form of small bubbles with transparent contents. In particular, photodermatosis, an “allergy” to solar radiation, which at an early stage looks like one of the forms of pyoderma, may manifest itself in infants.
To distinguish, you must gently press the rash element with your finger. If the rash is allergic in nature, the skin around the inflammation will lose its pink or red color. With streptoderma color after pressing remains the same.
Chickenpox
Sometimes the debut of varicella can be mistaken for the first stage of streptococcal inflammation of the skin: The rapid development of infection with chickenpox contributes to a fairly short-term differentiation from skin inflammation. If necessary, in both cases, you can apply a local antiseptic, zinc ointment to establish an accurate diagnosis.
Prevention of pyoderma caused by streptococcus
Streptococcal infections cannot be prevented, the prevalence of this pathogen is too high. However, you can increase the body’s resistance to contact with streptococci and reduce the likelihood of contact with active agents.
To enhance the immune protection of the child, you must first pay attention to the observance of sleep, rest and games, walks, study, as well as the usefulness of the diet rich in vitamins and minerals. From an early age, it is necessary to instill hygiene rules, wash hands, use personal dishes, towels, etc. Streptococcal resistance.
After the diagnosis of the disease, it is necessary to take measures to reduce the likelihood of streptoderma in contact with family members with the child. General hygiene measures and rules (cleaning, frequent replacement of clothes, bed linen, removal of soft toys, blankets from the patient’s room, individual dishes and towels) will help not only to preserve the health of relatives, but also to avoid long-term course and recurrence of pyoderma.
In order to prevent an outbreak of streptococcal infection in preschool and general education institutions, sick children are isolated from the team at the time of treatment, all children who have been in contact with the patient are quarantined for 10 days (the maximum incubation period of the disease) .