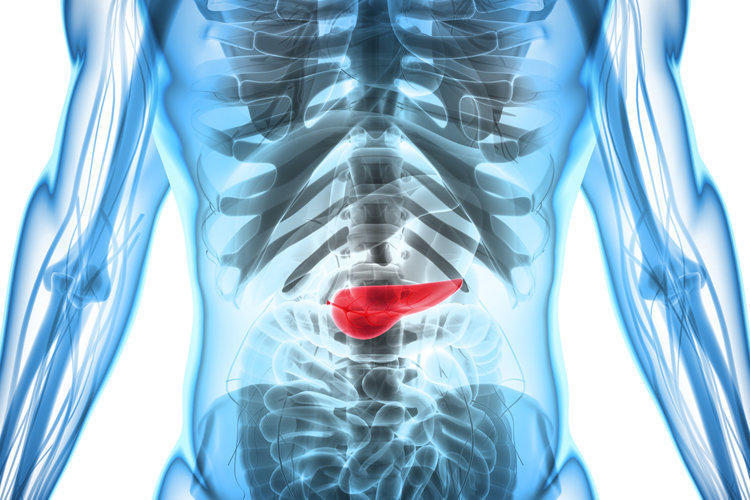
Diseases of the pancreas, its dysfunction and pathology have a pronounced effect on human well-being and overall human health. The main functions of the pancreas are the production of digestive enzymes and the production of insulin, a hormone that regulates the energy metabolism of glucose in tissues.
- Pancreas: symptoms of inflammatory disease
- Acute Pancreatitis
- Pain as a symptom of acute pancreatitis
- Dyspepsia for pancreatitis
- Features of nausea and vomiting as signs of acute pancreatitis
- Dehydration: severity of dehydration
- Functional bowel disorders
- Skin manifestations of pancreatic dysfunction
- Other symptoms
- Laboratory tests and indications for acute pancreatic inflammatory process
- Pancreas: symptoms of other diseases and pathologies
Pancreatic diseases are divided into the consequences of developmental disorders, injuries, inflammatory processes and malignant organ lesions. What are the symptoms of pancreatic disease? The clinical picture depends on the cause of the disease or pathology and the stage: acute or chronic, as well as on the individual characteristics of the patient. In diseases of the pancreas, symptoms may also vary depending on the age of the patient and the rate of metabolic processes, but do not correlate with gender: the symptoms of pancreatic disease in women and the symptoms of pancreatic disease in men are similar.
When self-diagnosing the presence of signs of diseases and destructive processes of the gland, it is necessary to remember that some inflammatory processes and dysfunctions have fairly similar symptoms, and the disease can only be determined using laboratory and instrumental examination methods.
Pancreas: symptoms of inflammatory disease
Non-infectious inflammatory processes in pancreatic tissues are the most common cause of dysfunctions and pathologies of this organ. Most of the processes of inflammatory nature are expressed by the clinical picture of pancreatitis, accompanied by swelling, disintegration and death of the glandular tissues.
Long-term inflammatory processes lead to the replacement of glandular tissue with connective tissue, impaired anatomical structure and pancreatic functions.
The primary inflammatory process of a non-infectious nature may be complicated by the layering of bacterial infections, the formation of cysts, inflammation of the peritoneum, internal bleeding and other complications of the disease. Depending on the symptoms and the clinical picture, acute and chronic types are distinguished pancreatitis .
Acute Pancreatitis
The most common cause of the development of acute pancreatitis is a complication of gallstone disease when the diet is broken, an excess of fatty foods, and alcohol. The average age of the first episode of acute pancreatitis is 40-50 years.
Among the types of diseases distinguish:
- acute interstitial (edematous) form of pancreatitis;
- acute hemorrhagic form;
- acute purulent form of pancreatitis;
- acute pancreatic necrosis with total or partial tissue death.
When the symptoms of pancreatitis on the background of cholecystitis are diagnosed, cholecystopancreatitis is diagnosed. Acute pancreatitis can manifest itself in a variety of ways and not have a pronounced, uniform clinical picture, which makes diagnosis difficult.

Pain as a symptom of acute pancreatitis
The acute form of the disease is always accompanied by pain. Depending on the edematous or necrotic variety, as well as on the involvement of organs and tissues of the peritoneum in the inflammatory process, the pain may be acute, dull, pulling, cutting, etc.
The edematous form of pancreatitis causes pain due to squeezing of the nerve endings by puffing-up tissues, stretching the organ capsule and blocking ducts.
Necrotization of tissues with pancreatic necrosis can cause such severe pain that it provokes a life-threatening condition – a painful shock.
Localized pain in the epigastric region, can spread throughout the abdomen and in most cases radiating to the spine, due to the location of the pancreas and the specifics of its innervation. In rare cases, differential diagnosis is required from manifestations of myocardial infarction and angina, as pain may occur behind the sternum, in the heart area, and radiating to the clavicle region.
Pain in acute pancreatitis does not correlate with food intake, being an expression of the inflammatory process and increasing pathological changes. Pain is prolonged or permanent, decreasing when taking painkillers and anti-inflammatory drugs.
Dyspepsia for pancreatitis
Dyspeptic symptoms of acute pancreatitis are expressed in nausea, vomiting after eating with inclusions of undigested food, impaired defecation: constipation, diarrhea, or alternation. Dyspeptic symptoms often occur in the initial stage of pancreatitis as a consequence of a violation of the diet. The most frequent “provocateurs” are fatty foods, alcohol, mushrooms, honey, tomatoes, and their processed products. Some medications are also capable of provoking the onset of the disease, in the number of drugs – drugs of antibiotic groups, sulfonamides, nitrofurans, cytotoxic drugs, etc.
Features of nausea and vomiting as signs of acute pancreatitis
In the vast majority of cases with pancreatitis, vomiting is preceded by a feeling of nausea, resulting from irritation of the so-called vagus nerve. 8 out of 10 bouts of nausea end with the release of vomit, not bringing relief to the patient.
Vomiting with pancreatitis – a sign of intoxication. At the first stage, the vomit consists of the contents of the stomach, with further development of the disease there are inclusions of bile, which indicates that the contents of the duodenum have been cast from the stomach. The volume of masses and the frequency of attacks depend on the stage of the disease and can be quite significant, severe, painful, leading to hypo-osmotic dehydration of the organism.
Dehydration: severity of dehydration
Dehydration in the absence of timely treatment develops from the initial stage to the threatening death. At the first stage, with the loss of less than 3% of body weight due to fluid withdrawal, patients feel weak thirst, the respiratory rate is somewhat increased.
At the second stage, with the loss of 3 to 9% of body weight, there is a pronounced sensation of thirst, dryness of mucous surfaces, symptoms of skin loss of moisture: skin gathered in a fold does not smooth out immediately, turgor is lowered. There is an acceleration of heart contractions, the volume of urine is reduced, its color becomes darker.
The third stage is accompanied by neurological manifestations (confusion of consciousness, slow reaction, drowsiness, speech disorders), lowering of blood pressure, disturbances of heart rhythm due to electrolyte imbalance, acidosis. This stage can lead to hypovolemic shock, the development of multiple organ failure and cessation of vital activity.
Functional bowel disorders
Violation of the production of pancreatic enzymes for the digestive process and a decrease in the secretion of bile acids lead to increased flatulence, bloating, flatulence at the initial stage of the inflammatory process in the pancreas. Enzyme and biliary insufficiency also cause prolonged constipation, absence of stool, or difficulty in the process of defecation for several days. Further, the absence of stool gives way to intestinal upset with feces of liquid consistency. Such periods of stool retention and dilution are characteristic of pancreatitis.
Skin manifestations of pancreatic dysfunction
The inflamed pancreas, due to the swelling of the organ, puts pressure on the surrounding organs, most often preventing the outflow of bile, which is manifested by paleness or yellowness of the skin.
With pronounced respiratory disorders, oxygen deficiency, cyanosis of the nasolabial triangle, nails on the hands and feet is noted. Spots of a cyanotic color can also appear on the abdomen near the navel or on the sides.
Other symptoms
There is also increased salivation, tachycardia, a number of symptoms, allowing to diagnose pancreatitis during palpation, such as:
- pain on palpation of the angle between the ribs and the spine on the left side;
- pain when pressed 2 cm under the umbilical fossa inward and upward;
- increased pain after pressing on the stomach, at the time of the removal of hands.
Laboratory tests and indications for acute pancreatic inflammatory process
The main diagnostic value are indicators of blood. Characteristic changes in the acute form of pancreatitis are leukocytosis as a sign of an inflammatory process and an increase in the level of amylase.
The normal serum amylase content is 65 units, with an increase in the reference index twice acute pancreatitis is considered as a probable diagnosis. 1000 units are considered a critical concentration of amylase, this condition is regarded as life-threatening and requires emergency surgical care.
Despite the high diagnostic value of amylase indicators, its compliance with the norm is not an accurate marker of the absence of an inflammatory process. In the first hours of the development of an acute form of the disease, as well as at the stage of tissue necrosis, the level of amylase may be normal.
When deciphering the analyzes, they are also guided by the indicator erythrocyte sedimentation rate, hematocrit, reference values for glucose, lipase, trypsin, pancreatic enzyme inhibitors and elastase.
Pancreas: symptoms of other diseases and pathologies
Diseases and dysfunctions affecting the pancreas are not limited to inflammatory processes. Although the majority of pathologies are characterized by pain, dyspeptic symptoms and features of the blood formula, symptoms vary depending on the type of disease, its form, stage and extent of pathology.
Laboratory research is not very informative. Ultrasound, biopsy Exceeding the reference norms of glucose and glycated hemoglobin in the blood
| Disease / symptom | Chronic pancreatitis | Cancer | Cystic changes in glandular tissue | Type I Diabetes |
| Pain | In periods of exacerbations | Depending on the location and volume of the tumor | Depending on size and location, may be missing | None |
| Dyspepsia | During periods of exacerbation and in violation of the diet: constipation, diarrhea, nausea, vomiting | Unsustainable fatty stools, nausea, at the late stage – profuse diarrhea, vomiting | Depending on the location of the cyst: rapid stool, bloating (cyst on the gland head), constipation, nausea, discolored feces (body, tail of the gland) | Feeling nauseous, vomiting with ketoacidosis. Excessive hunger in hypoglycemia |
| Features of the clinical picture | Exacerbations in case of violation of dietary rules | Yellowness, pallor of the skin, weight loss before exhaustion | Expressed in late stages and bacterial suppuration with pain and the possibility of palpation of cysts | Increased thirst, frequent urination, pruritus, dry mucous membranes. Ketoacidosis, hypoglycemia |
| Laboratory values and diagnostic methods | For exacerbations similar to acute pancreatitis | In the blood picture – anemia, leukocytosis, increased ESR. Ultrasound, biopsy |
Ulcerative changes in the glandular tissue of this organ are classified depending on the stage: erosive, exacerbation and chronic, with possible complication of penetration into the tissue and organs of the peritoneum. The symptoms of the ulcer are similar to the clinical picture of pancreatitis with heartburn and salivation supplements.
Therapy is carried out under the strict supervision of specialists. During treatment, it must be remembered that without dieting, restrictions on fatty, fried, smoked foods, certain types of foods (mushrooms, tomatoes, honey) and alcoholic beverages, the disease will worsen and progress.