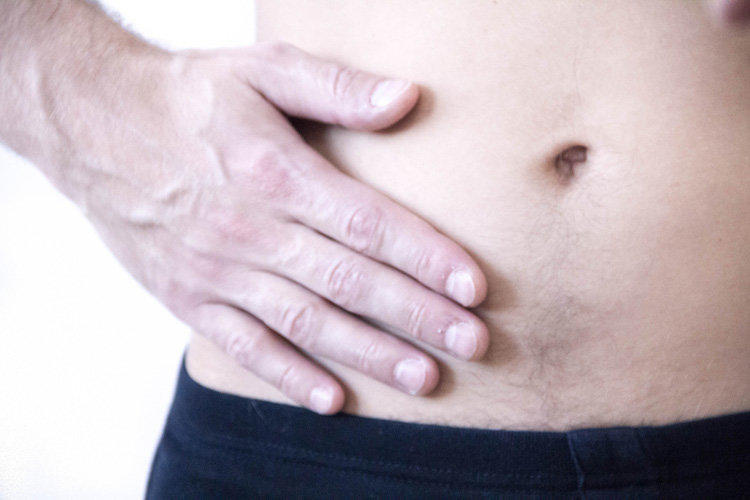
Appendicitis is the most common surgical disease of the digestive system, and one of the most dangerous. The danger of the disease lies primarily in its transience and the inevitability of serious, life-threatening complications. The probability of encountering acute appendicitis during life is quite high. It is diagnosed in 5-10% of people.
Appendicitis can occur at any age and in people of any gender. However, statistics show that most often it is inflamed in people aged 5-40 years. Among the patients aged 20–40 years, there are twice as many women as men, while among patients under the age of 20 years, men predominate. Women in general are ill more often than men. After 40 years the probability of occurrence of the disease is significantly reduced, but does not become zero. Therefore, appendicitis can occur in the elderly. Also, appendicitis is rarely diagnosed in children under 5 years of age.
Description of the disease
Appendicitis is an inflammation of the appendix, the appendix located in the lower part of the intestine. In the normal state, the appendix is a small tube with a diameter of 7-10 mm and a length of 50-150 mm. It branches off from the cecum, while gradually narrowing, and does not have a through passage.
The function of the appendix is not precisely clarified. Previously, an appendix was considered as a simple rudiment, borrowed by man from his distant ancestral animals with a herbivorous diet and now functionally useless. Now there is good reason to believe that it plays an important role in endocrine and immune processes, as well as in the formation of intestinal microflora. It is proved that people with a remote appendix have problems with a sufficient number of beneficial microorganisms in the intestine. However, the appendix is not among the vital organs without which the body can not exist.
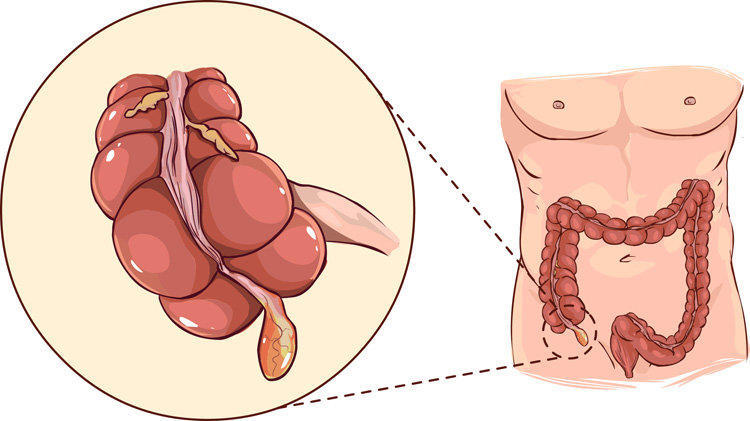
Generally, inflammation of the appendix is acute. As a result of the disease, pus accumulates in the appendix, which cannot freely leave due to the narrowness of the appendix. The appendix grows in size and becomes painful. Ultimately, this leads to rupture of the wall of the Appendix and the release of pus to the outside. This, in turn, entails acute peritonitis (inflammation of the peritoneum), sepsis or abscesses in the abdominal cavity, which with a high degree of probability can be fatal. The most serious complication is pylephlebitis – the portal vein inflammation resulting in severe liver damage, with a particularly high lethality.
The disease is very fast and usually lasts no more than 2-4 days, rarely more than a week. Cases of spontaneous treatment of acute appendicitis are infrequent. Sometimes a protective infiltration of surrounding tissues may form around the affected appendix, but this formation can also lead to an abscess. Therefore, the disease requires medical intervention and surgical treatment. With timely treatment of the disease, the prognosis is favorable.
Occasionally, there is also chronic appendicitis, which is characterized by appearing now and then retreating symptoms common for acute appendicitis. The frequency of occurrence of this condition is about 100 times less than that of an acute one. As a rule, it does not require surgical treatment.
Acute appendicitis is divided into simple (catarrhal) and destructive, fraught with complications. Without proper treatment, simple appendicitis almost always becomes destructive.
The main stages of appendicitis:
- Catarral
- Phlegmonic
- Gangrenous
- Perforated
Causes
The causes of appendicitis in adults have not yet been precisely determined. However, scientists agree that there is no single cause of appendicitis common to all patients. Every patient can have a reason of his own. In most cases, appendicitis is caused by blockage of the entrance of the appendix into the rectum. The causes of blockage can be different – for example, ingress of fecal stones or foreign bodies into the process. It can also be caused by squeezing the upper part of the process due to adhesive processes resulting from cholecystitis or enteritis.
Bacteria – enterococci, streptococci, staphylococci and E. coli also play a big role in appendicitis. Most often there is a combination of both of these factors. The stagnation of the contents of the process leads to a weakening of its internal immunity and the introduction of pathogenic bacteria into the mucosa. There is also a theory that the main cause of appendicitis is a spasm of the vessels that feed the appendix with blood. Another possible cause is injuries to the abdomen that caused damage or movement of the process.
The factors contributing to the disease should include a tendency to constipation, poor intestinal motility, lack of vegetable fiber in food, overeating, many infectious diseases of the gastrointestinal tract, the presence of parasites. Hereditary factors can also affect the appearance of the disease, as well as reduced immunity due to bad habits, stress, lack of vitamins and trace elements.
Also marked by an increased incidence of appendicitis in pregnant women – due to the displacement of the process caused by an increase in the size of the uterus. In the case of some diseases of the uterus, it is possible to transfer the focus of inflammation to the appendix.
Symptoms

For the early diagnosis of appendicitis, symptoms are essential. Their knowledge allows you to cut off other gastrointestinal diseases that are not related to the inflammation of the appendix.
The main signs of appendicitis in adults include:
- Acute abdominal pain, including with pressure
- Temperature increase
- Nausea
- Vomiting
The first symptoms and signs of acute appendicitis do not always allow to uniquely identify this disease. Initially, the disease may be masked as another, not so dangerous, and a person may take an attack of appendicitis for renal colic or gastritis.
The main symptom of appendicitis is persistent acute pain in the abdomen. As a rule, a sharp pain appears unexpectedly, most often at night or in the morning. In the catarrhal stage, pain is first spread throughout the abdomen or appears in its upper part (in the epigastric region). But then the pain concentrates in the right lower abdomen, below the navel and just above the thigh (in the iliac region).
The process of moving the focus of pain is called Kocher’s symptom and is one of the main determining signs of the disease. In most cases, it testifies to appendicitis, and not to any other disease of the gastrointestinal tract. This process occurs within a few hours after the onset of the disease. The nature of the pain also changes over time, it intensifies, becomes pulsating and aching. The pain is aggravated by laughing and coughing, taking a deep breath, subsides a little when turning to the right side or in a position where the legs are folded towards the stomach. The pain may also irradiate to the right leg and be felt when walking. When pressing on the iliac region, the pain is usually almost not felt, but if you abruptly release the abdomen, then there is severe pain. There is tension in the abdominal wall.
With the development of the disease, the pain may subside for a while. But this does not indicate a cure, but only a necrosis of the tissues of the wall of the process, including its nerve endings. However, pressure on the iliac region is still extremely painful. After this stage, perforation of the wall usually occurs, pus spreads through the peritoneum and the pain returns, intensified many times.
It should be borne in mind that sometimes the appendix may be located on the left, so in this case the left side of the abdomen will hurt. In some cases, pain can be felt in the right hypochondrium, in the pubic, pelvic, lower back area.
Symptoms of appendicitis in adults also include disorders of the gastrointestinal tract. First of all, it’s nausea. Sometimes there may be vomiting and diarrhea, not bringing relief. However, diarrhea in appendicitis is characteristic, above all, for children, in adults it is less common. There are also delayed stools, a feeling of dry mouth. In case of non-standard position of the appendix, urinary retention (dysuria) may appear. Tachycardia is often noted – up to 90-100 beats per minute.
In the initial phase of the disease, the temperature rises slightly – up to + 37-38 ºС. Subsequently, the temperature may even fall to normal, but in the final stage, preceding the outbreak of pus out, it again rises to high rates – + 39-40 ºС. In this case, the pain is significantly increased.
In the case of appendicitis in the elderly, its symptoms can be erased and invisible until the disease goes into a destructive stage. The pain may be dull, the nausea may be minor, and such a feature as fever may be absent altogether. However, this does not mean that appendicitis is easier in older people. On the contrary, in the elderly, complications of appendicitis are much more common.
Diagnosis of appendicitis is also difficult in young children (under 5 years of age). This is due to the fact that the signs of appendicitis in adults are usually more pronounced than in children. Sometimes appendicitis in a child is masked as a simple indigestion. The pain is often not localized in the iliac region, and sometimes the child can not explain exactly where he has a stomach ache. In this case, one should be guided by such signs as a temperature rise to +38 ºС, a coated tongue, diarrhea. However, all these symptoms may occur with other diseases, so the child must be shown to a specialist.
Atypical forms of appendicitis
There are also several forms of atypical appendicitis, in which the symptoms may differ from the standard ones.
- Emipiema. A form of appendicitis with slow development, in which the Kocher symptom is absent and pain immediately appears in the iliac region.
- Retrocecal appendicitis. It is characterized by weak signs of peritoneal inflammation, loose stools. Pain is often felt in the lumbar region and radiates to the hip area.
- Left-sided appendicitis. It has a classic clinical picture, but pain is felt in the left iliac region.
- Pelvic appendicitis. More characteristic of women. There is a slight fever, dysuria, pain radiating to the navel.
What should I do if I suspect appendicitis?
At the slightest suspicion of appendicitis should call a doctor. The reason for going to a doctor is any persistent abdominal pain that does not go away for 6 hours. You should not take laxatives, antibiotics or other gastrointestinal medications, and especially analgesics, before a doctor’s examination, since all these drugs can blur the clinical picture and make it difficult to make a diagnosis. It is also prohibited to install a heating pad on the right side of the abdomen, since an external heat source can accelerate the development of the disease. Shows bed rest. Should refrain from eating. When the doctor comes, you need to tell him about all the symptoms, about how a stomach ache, and allow him to carry out an examination.
Diagnostics
For diagnostic purposes, visual inspection and palpation are primarily used. The main symptoms are strained abdomen, pain in the lower right. However, these methods are not always reliable. Such diagnostic methods as ultrasound, MRI and computed tomography, blood and urine tests are also used. When viewing a blood test, the main attention is paid to the increased level of leukocytes in the blood (leukocytosis). Diagnostic laparoscopic examination can also be performed through an opening in the abdominal wall.
It should be noted that the recognition of the disease can be difficult, because the symptoms of acute appendicitis are in many ways similar to other diseases of the gastrointestinal tract. These include acute gastroenteritis, pancreatitis, an ulcer (especially if it is perforated), intestinal or renal colic, inflammation of the uterus, stretching or tearing of the abdominal muscles. Therefore, it is important to differentiate appendicitis from other diseases, which for the most part do not require urgent surgical intervention.
Treatment
Appendicitis is usually treated surgically. It consists in removing the appendix (operation of appendectomy). In some cases, it may be preceded by therapy with antibiotics. Sometimes it is possible and conservative treatment, without removal of the process – in this case, prescribe antibiotics. As a rule, it is resorted to if there are any contraindications to the operation.
Surgery to remove the process is carried out either in the traditional way, using an open incision, or by laparoscopic method. The first 12 hours after surgery, you should observe bed rest and avoid eating. During the recovery period, it is also possible to treat the effects of the disease with antibiotics. The duration of the recovery period depends on what stage of the disease the operation was performed and usually takes 1-2 weeks.