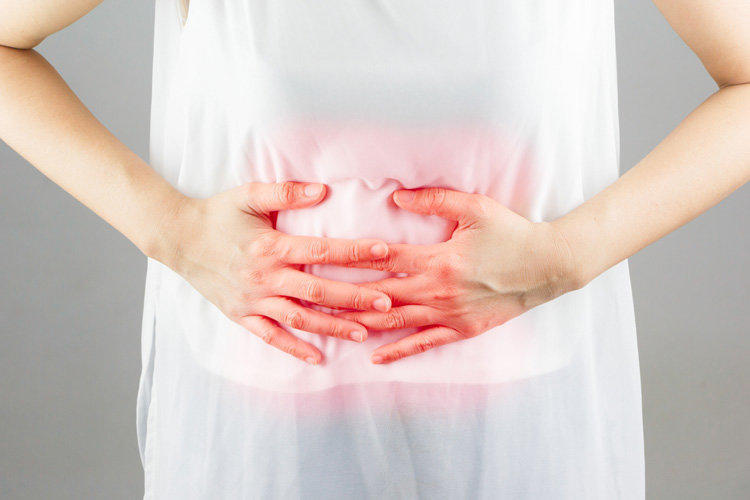
This is one of the most common diseases on Earth. According to statistics, about one in four people suffer from irritable bowel syndrome (IBS). However, only one in three of their number appeals for help. The disease is also known as bowel neurosis or irritable bowel syndrome.
Description and causes of the disease
Compared to other diseases of the gastrointestinal tract, irritable bowel syndrome stands apart. After all, it would seem that nothing can provoke him. In patients with IBS, there is no damage to the intestinal mucosa by pathogenic microorganisms, as well as any pathology of the tissues of the intestinal tract of inorganic origin. And, nevertheless, the disease manifests itself, and sometimes numerous examinations can not establish what actually happens to the human body.
Now the prevailing point of view in medical science is that in most cases the immediate cause of irritable bowel syndrome is stress. This is confirmed by the fact that anxiety, depression and other neurotic disorders occur in approximately 60% of patients with IBS.
To understand why this is happening, you need to understand the mechanism of the intestine. The main functions of the large intestine – absorption of water and minerals from food debris, the formation of feces and their promotion to the rectum. The latter tasks are accomplished thanks to the contraction of the muscle walls and the secretion of mucus.
It may seem surprising to many, but the intestines do not always work by themselves, in a completely autonomous mode. The intestine has its own nervous system, which is called the enteric. It is part of the autonomic nervous system and is not directly dependent on the central nervous system. However, the regulatory regions of the brain are responsible for the production of substances that control the work of the autonomic nervous system, including the intestinal nervous system. This relationship is called the intestine-brain axis and is bilateral. And under stressful situations, failures in the functioning of this mechanism begin. The brain gives the wrong signals to the intestines, and that, in turn, incorrectly informs the brain about the processes occurring in it. There is a violation of intestinal motility, the slightest discomfort in the intestine causes bouts of pain. This is due to another important circumstance in which the disease develops – an increased level of sensitivity to pain.
However, stress and a low pain threshold are most often not the only factors causing the disease. In most cases, there is a whole complex of reasons.
Circumstances contributing to irritable bowel syndrome:
- Dysbacteriosis
- Irregular and unbalanced nutrition
- Sedentary, sedentary work
- Genetic predisposition. It has been established that the majority of IBS sufferers have close relatives who also had a similar disease.
- Disruption of hormonal levels in women (for example, during pregnancy or during menstruation)
An important role in the occurrence of irritable bowel syndrome is played by the nutritional factor. There are certain categories of products, the frequent use of which contributes to the emergence of IBS. These products include:
Also, IBS can be observed after completing the treatment of certain infectious bowel diseases. This type of irritable bowel syndrome is called post-infectious.
Among the factors causing IBS, sometimes referred to as excessive growth of microflora. However, beneficial microorganisms can not cause by themselves problems with the intestines and scientific evidence of their connection with the occurrence of IBS does not exist. Another thing is the growth of pathogenic microorganisms, however, such diseases are infectious and require very different approaches and treatment methods.
Irritable bowel syndrome is almost two times more common in women than in men. Perhaps this is due to the greater emotionality of the weaker sex, as well as the fact that women often have changes in the level of hormones. It is also possible that women simply tend to go to doctors more often. IBS is a disease of predominantly middle age, since the highest incidence of the disease occurs at the age of 25-40 years. In older people (over 60), the disease is much less common.
In children and adolescents, irritable bowel syndrome is also not uncommon, but accurate statistics on this score does not exist. Often, children with IBS do not pay attention, taking it for intestinal infectious disorders. Many experts believe that cases of irritable bowel syndrome detected in adulthood are formed in childhood.
Symptoms of irritable bowel syndrome
Irritable bowel syndrome is characterized by chronic symptoms such as increased gas formation (flatulence), bloating, constipation, diarrhea (diarrhea), pain and colic in the lower abdomen. Approximately every third disease, accompanied by similar symptoms – is IBS. An important feature is that the discomfort in the abdomen, as a rule, appears after eating and disappears after defecation.
Pains are usually cramping (spastic). However, there may be pain and whining or piercing types.
Also, the disease is characterized by signs such as discharge of mucus from the stool, a change in stool consistency, irresistible or false urge to have a bowel movement, a feeling of incomplete bowel movements after bowel movements.
There are three main types of irritable bowel syndrome:
- Accompanied by diarrhea (approximately 2/3 of the total number of patients)
- Constipated (about a quarter)
- Combining constipation and diarrhea (less than 10%)
In some cases, changes in stool are not observed, and all the symptoms of irritable bowel syndrome are reduced to increased flatulence and intestinal colic.
By diarrhea, it is customary to imply a bowel movement that occurs at least three times a day. As a rule, people suffering from this type of disease feel the urge in the morning or in the morning. At night, the urge is usually absent. Also, diarrhea often begins in case of stress or strong experiences. This syndrome is sometimes called “bear disease.”
Constipation is considered a chair that happens no more than once every three days. Constipation can also be accompanied by symptoms such as dyspepsia, nausea, dry mouth. There may be colic in front of the stool, which disappears after a bowel movement.
Patients also have vegetative disorders such as headaches, insomnia, chronic fatigue syndrome. Irritable bladder syndrome (almost a third of cases) may also occur.
Diagnostics
If you have found symptoms similar to IBS symptoms, it is recommended to be examined. It is best to consult a gastroenterologist. Diagnosing IBS is not an easy task. Usually, IBS is diagnosed if all the attempts to find any infectious agents or bowel pathologies in analyzes or research results fail.
It is also important to consider the frequency of symptoms and the duration of the period during which they are observed. The world’s leading gastroenterologists have proposed the following criteria. It is believed that IBS include stool disorders that occur at least 3 days a month. They should also be observed for 3 consecutive months. The relationship between the onset of symptoms and the change in the frequency and appearance of the stool should also be taken into account.
When diagnosing, it should be separated from IBS diseases such as:
- infectious diseases of the digestive tract
- helminthic invasions
- dysbacteriosis
- anemia
- beriberi
- tumors
- polyps
- ulcerative colitis
- short bowel syndrome
- intestinal tuberculosis
- Crohn’s disease
Disorders of the bowel, reminiscent of IBS, may also be characteristic of some forms of diabetes, thyrotoxicosis, carcinoid syndrome. Disorders of the bowel in old age require particularly careful examination, since for older people IBS is generally not typical.
It is also not worth mixing individual cases of gastrointestinal disorders with IBS that can occur in healthy people after heavy meals, drinking large amounts of alcohol, carbonated drinks, unusual or exotic food, for example, while traveling.
Signs such as fever, the acute nature of the symptoms or their increase over time, night pain, bleeding, persistent for several days, lack of appetite, weight loss, for IBS are not typical. Therefore, their presence indicates some other disease.
When diagnosing, it is necessary to do the following tests:
- Complete blood count
- Biochemical blood test
- Stool analysis (coprogram)
- Blood test to the reaction to gluten
The methods of colonoscopy and irrigoscopy, esophagogastroduodenoscopy, and ultrasound of the abdominal cavity are used to exclude colon pathologies. In some cases, can be used and biopsy of the intestinal wall. In case of severe pain syndrome, the doctor may offer to undergo electrogastroenterography, manometry, and balloon dilatation test.
When the tendency to diarrhea is being tested for tolerance to lactose and the analysis of intestinal microflora. If diarrhea is absent, a radioisotope transit study may be used. After completing the initial course of treatment, some diagnostic procedures can be repeated in order to establish the degree of effectiveness of therapy.
Treatment of irritable bowel syndrome

Full recovery from the disease is difficult due to the fact that, as a rule, it is caused not by one cause, but by their complex. In addition, medicine has not yet established the exact mechanism for the development of the disease, so the treatment regimen for irritable bowel syndrome in general does not exist. But this does not mean that it is completely unknown how to treat and how to treat the disease. Practice shows that irritated intestines can be cured in about a third of cases, and in others it is possible to reduce the degree of symptoms.
On the other hand, irritable bowel syndrome can not be called a disease that threatens life and health. Irritation of the intestine gives patients a lot of trouble, but usually does not in itself lead directly to any complications, dysfunctions and damage to the tissues of the gastrointestinal tract.
Many people who have been diagnosed with IBS, gradually get used to their symptoms and are treated independently, or adjust their lifestyle so that the disease would not interfere with it.
However, the disease should not be ignored, and symptomatic treatment of the disease is more than desirable. After all, such symptoms of IBS as frequent diarrhea and constipation are far from harmless, since they create an increased load on the rectum and can lead to diseases such as hemorrhoids, fissures in the anus and paraproctitis. This is especially true for constipation. Diarrhea in addition also contributes to dehydration. Also, do not ignore the hidden causes of the disease – anxiety and depressive states, which can lead to much more serious problems with the body.
But the most important thing is that the attacks of pain and stool disorders lead to a decrease in the quality of life. In case of sudden onset of illness, a person may have problems with performing his work duties or communicating with other people. All this further aggravates the stressful state of a person, which creates a kind of vicious circle from which it is becoming increasingly difficult to get out. With IBS treatment is always conservative. It may include both drug and non-drug methods.
Diet
The main non-drug treatment method is diet. Diet with IBS should not be strict. First of all, it should be aimed at systematization and ordering of the nutrition process, giving it a regular character, as well as at improving the balance between various products. Food should be taken in small portions, overeating should be avoided.
Selection of the diet depends on what type of disease is observed in the patient. If diarrhea prevails, the proportion of foods that cause them – for example, fruits and vegetables, dairy products – should be reduced in the diet. If constipation is most often observed, then you should limit the amount of fatty and salty foods. Constipation is also recommended to consume more water. People suffering from flatulence, it is necessary to limit the use of carbonated beverages, legumes. But it hardly makes sense to abandon some types of products, especially vegetables and fruits, completely.
Sometimes there are recommendations to add more plant fiber to food. However, many scientists believe that following these guidelines does not reduce the intensity of the symptoms. Moreover, in the case of IBS with diarrhea, increased fiber consumption can only strengthen them. Of course, it is not necessary to completely abandon fiber, since it plays an important role in the proper functioning of the intestine and in the prevention of many diseases, but a mechanical increase in its consumption does not make much sense.
In general, the diet should be selected on an individual basis. A diet suitable for one patient does not always help another. Therefore, it is better to note after which products the occurrence of unpleasant sensations and symptoms is most often observed and to exclude them from the diet. Consultation with a professional nutritionist will also be helpful.
Preparations
Drug treatment of irritable bowel syndrome is mainly symptomatic.
The main groups of drugs:
- Antispasmodics
- Defoamers
- Anti-diarrheal drugs (for a disease with persistent diarrhea)
- Laxatives (for the case of persistent constipation)
- Intestinal microflora regulators (probiotics and prebiotics)
Antidepressants and tranquilizers are used to eliminate the mental causes of the disease. However, not every type of depressants is suitable in the case of irritable bowel syndrome. Tricyclic antidepressants, such as amitriptyline, demonstrated the greatest efficacy in the disease. Serotonin reuptake inhibitors, such as fluoxetine, can also be used. In some cases, benzodiazepines are recommended. But drug psychotherapy is a difficult branch of medicine, so the choice of drugs can only be done by a qualified psychotherapist. Independent selection of psychotropic drugs can lead not only to the deterioration of the intestine, but also to the aggravation of neurological problems – depression or anxiety.
In some cases, light sedatives are also effective, based on plant components – Valerian and Leonurus. They have a minimum of side effects and therefore they can be used safely.

When exacerbating the disease, there are many ways to soothe the intestines. As a remedy for diarrhea, such a common drug as Imodium, or its structural analogue containing loperamide, is best suited. The action of the drug is based on slowing the movement of food through the intestines. Sorbents can also be used, such as Smekta .
But for the treatment of constipation caused by the disease, not every laxative will do. It is best to use laxatives for this purpose, the effect of which is based on an increase in the volume of fecal masses and an increase in their water content. These drugs are usually made on the basis of plantain seed extract (Metamucil) or synthetic cellulose (Citrucel). They are not recommended to take before bedtime, as this may cause bloating. Laxative preparations based on senna and aloe are not recommended, as they can increase the volume of gas and increase abdominal pain.
Antifoaming agents are intended for the treatment of flatulence – drugs that reduce the amount of gas in the intestine. As a rule, they are based on simethicone and dimethicone. Among such drugs, Meteospasmil, Polysilan, Zeolat, Espumizan can be noted.
Antispasmodics are best suited for flatulence and imperative urge to defecate. To reduce spasms and associated pain, traditional universal antispasmodics can be used like No-shpa (Drotaverine). It is also worth paying attention to specialized antispasmodics used to treat spasms in the digestive tract, for example, Duspatalin. Suitable for relieving spasms and drugs from the group of blockers of m-cholinergic receptors (Buscopan). When using muscle relaxant muscle relaxants should be borne in mind that they are contraindicated in pregnancy.
Dysbacteriosis is a syndrome that, as a rule, accompanies the disease and results in a decrease in the amount of beneficial intestinal microflora. It is usually characteristic of the diarrheal type of the disease.
To correct the situation, probiotics (preparations containing organisms of the intestinal microflora) or prebiotics (preparations that improve the habitat of the microorganism) are used.
Among probiotics, it is preferable to use products containing lactic acid bacteria Bifidobacterium infantis or Sacchromyces boulardii fungi, for example Linex and Enterol.
Traditional medicine also has many ways to combat intestinal disorders. Herbal preparations based on mint leaves, chamomile flowers and valerian root. When diarrhea, plantain, walnut, sage and blueberry are used, for constipation, yarrow, licorice root, and buckthorn bark.
Other measures
Exercise is one of the secondary methods of treatment. They improve the psycho-emotional state, as well as stimulate the contractile ability of the intestine. The type of exercise can be different and should be selected on an individual basis. Someone will be enough simple morning exercises or daily walks. Simulators, swimming can also be used. Studies show that more than half of the patients who began to engage in physical exercise on average half an hour or an hour per day soon experienced a decrease in the symptoms of the disease.
Also, the patient needs to improve the daily routine, to establish a normal sleep. Bed rest for the disease is contraindicated, since it can only worsen the patient’s mental state. It is also necessary to find out exactly which stressful situations can cause exacerbation of symptoms and, if possible, avoid them.
If stress is the basis of the disease, then psychotherapy is added to the non-drug methods of treatment. It can include hypnosis, relaxation sessions, psychological training and auto-training.