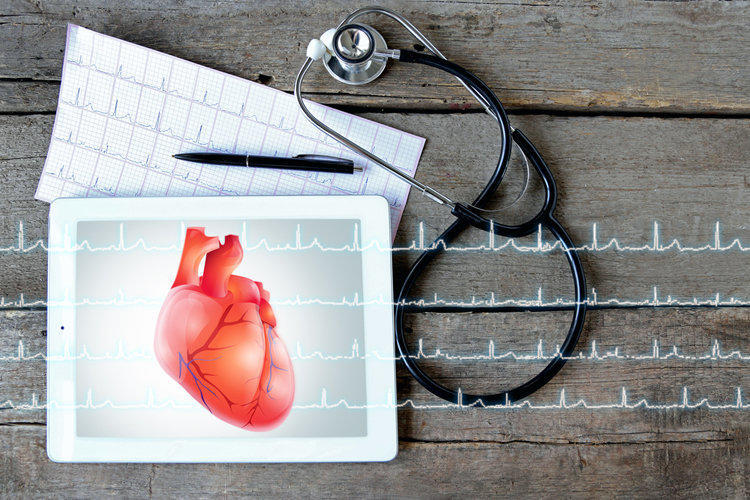
Electrocardiogram is a diagnostic method that allows you to determine the functional state of the most important organ of the human body – the heart. Most people have at least once in their life dealt with a similar procedure. But having received the result of an ECG, not every person, except that having a medical education, can understand the terminology used in cardiograms.
- What is cardiography
- Where can I make a cardiogram?
- Procedure Procedure
- Holter Monitoring
- Other types of procedures
- Recommendations for the standard procedure
- Tooth Types
- Major abnormalities and diagnosis
- Table of parameters of the cardiogram of an adult
- The norm of the duration of the elements of the cardiogram of a child
- The rhythm of contractions
- Heart Rate
- Heart Rate Types
- Atrial rhythm
- Atrioventricular rhythm
- Ventricular rhythm
- The electrical axis of the heart
- What do the findings on cardiograms mean?
- Atrioventricular block
- Ectopic rhythm
- Sinus bradycardia or tachycardia
- Non-specific ST-T changes
- Disorders related to conduction inside the ventricles
- Incomplete blockade of the right bundle of his bundle (NBPNPG)
- Complete blockade of the right bundle of His (PBNPG)
- Blockade of the anterior branch of the left bundle of His (BPVLNPG)
- Blockade of the posterior branch of the left bundle of His (B3VLNPG)
- Metabolic changes
- Low ECG Voltage
- Paroxysmal tachycardia
- Atrial fibrillation
- Sinoatrial blockade
- Hypertrophic myocardial conditions
- Myocardial Hypertrophy
- Left ventricular hypertrophy
- Right ventricular hypertrophy
- Left atrial hypertrophy
- Right atrial hypertrophy
- Normocardia
- Nonspecific T-wave changes
- Tachysystole
- ST Heart Depression
- Edge ECG
- Pathological ECG
- Ischemic ECG changes
- Decoding ECG in children
- ECG example with transcript
What is cardiography
The essence of cardiography is the study of electrical currents arising from the work of the heart muscle. The advantage of this method is its relative simplicity and accessibility. A cardiogram, strictly speaking, is called the result of measuring the electrical parameters of the heart, displayed in the form of a time schedule.
The creation of electrocardiography in its present form is associated with the name of the Dutch physiologist of the early 20th century, Willem Einthoven, who developed the basic ECG methods and terminology used by doctors today.
Thanks to the cardiogram, you can get the following information about the heart muscle:
- Heart rate,
- Physical condition of the heart,
- Arrhythmias,
- The presence of acute or chronic myocardial damage,
- The presence of metabolic disorders in the heart muscle,
- Electrical conduction disturbances,
- Position of the electrical axis of the heart.
Also, an electrocardiogram of the heart can be used to obtain information about certain vascular diseases not associated with the heart.
An ECG is usually performed in the following cases:
- Feeling abnormal heartbeat;
- Attacks of shortness of breath, sudden weakness, fainting;
- Pain in the heart;
- Heart murmurs;
- Worsening condition of patients with cardiovascular diseases;
- Medical examination;
- Clinical examination of people over 45;
- Inspection before surgery.
Also, an electrocardiogram is recommended when:
- Pregnancy;
- Endocrine pathologies;
- Nervous diseases;
- Changes in blood counts, especially with increasing cholesterol;
- Aged over 40 years (once a year).
Where can I make a cardiogram?
If you suspect that your heart is not all right, then you can turn to a general practitioner or cardiologist so that he would give you an ECG referral. Also on a fee basis, a cardiogram can be done at any clinic or hospital.
Procedure Procedure
ECG recording is usually performed in the supine position. To remove the cardiogram, use a stationary or portable device – an electrocardiograph. Stationary devices are installed in medical institutions, and the portable ones are used by emergency teams. The device receives information about the electrical potentials on the surface of the skin. Electrodes attached to the chest and limbs are used for this.
These electrodes are called leads. On the chest and limbs is usually set to 6 leads. Chest leads are designated V1-V6, limb leads are called the main (I, II, III) and reinforced (aVL, aVR, aVF). All leads give a slightly different picture of the oscillations, but by summing up the information from all the electrodes, you can find out the details of the work of the heart as a whole. Sometimes additional leads are used (D, A, I).
Typically, the cardiogram is displayed as a graph on paper media containing millimeter markings. Each lead-electrode has its own schedule. The standard belt speed is 5 cm / s; another speed can be used. The cardiogram displayed on the tape can also indicate the main parameters, the indicators of the norm and the conclusion generated automatically. Also, data can be recorded in memory and on electronic media.
After the procedure, it is usually necessary to decipher the cardiogram by an experienced cardiologist.
Holter Monitoring
In addition to stationary devices, there are also portable devices for daily (Holter) monitoring. They attach to the body of the patient along with the electrodes and record all the information coming in over a long period of time (usually during the day). This method gives much more complete information about the processes in the heart as compared with a conventional cardiogram. So, for example, when removing a cardiogram in a hospital, the patient should be at rest. Meanwhile, some deviations from the norm may occur during exercise, during sleep, etc. Holter monitoring provides information about such phenomena.

Other types of procedures
There are several other methods of conducting the procedure. For example, it is monitoring with physical activity. Deviations from the norm are usually more pronounced on an ECG with a load. The most common way to provide the body with the necessary physical activity is a treadmill. This method is useful in cases where pathology can manifest itself only in the case of intensive work of the heart, for example, in cases of suspected ischemic disease.
With phonocardiography, not only the electrical potentials of the heart are recorded, but also the sounds that arise in the heart. The procedure is assigned when it is necessary to clarify the occurrence of heart murmurs. This method is often used for suspected heart defects.
Recommendations for the standard procedure
It is necessary that the patient is calm during the procedure. Between physical activity and the procedure must pass a certain period of time. It is also not recommended to undergo the procedure after eating, drinking alcohol, drinks containing caffeine, or cigarettes.
Causes that can affect the ECG:
- Time of day,
- Electromagnetic background,
- Exercise,
- Eating,
- Electrode position.
Tooth Types
First you need to tell a little about how the heart works. It has 4 chambers – two atria, and two ventricles (left and right). The electrical impulse, due to which it is reduced, is formed, as a rule, in the upper part of the myocardium – in the sinus pacemaker – the nerve sinoatrial (sinus) node. The impulse spreads down the heart, first touching the atria and causing them to contract, then the atrioventricular ganglion and the other ganglion, the bundle of His, pass and reach the ventricles. It is the ventricles, especially the left one, involved in the great circulation that take the main burden of blood pumping. This stage is called contraction of the heart or systole.
After the reduction of all parts of the heart, it is time to relax – diastole. Then the cycle repeats over and over again – this process is called a heartbeat.
A heart condition in which there is no change in the propagation of impulses is reflected on the ECG as a straight horizontal line, called isoline. The deviation of the graph from the contour is called a tooth.
One heartbeat per ECG contains six teeth: P, Q, R, S, T, U. The teeth can be directed both up and down. In the first case, they are considered positive, in the second – negative. The Q and S teeth are always positive, and the R wave is always negative.
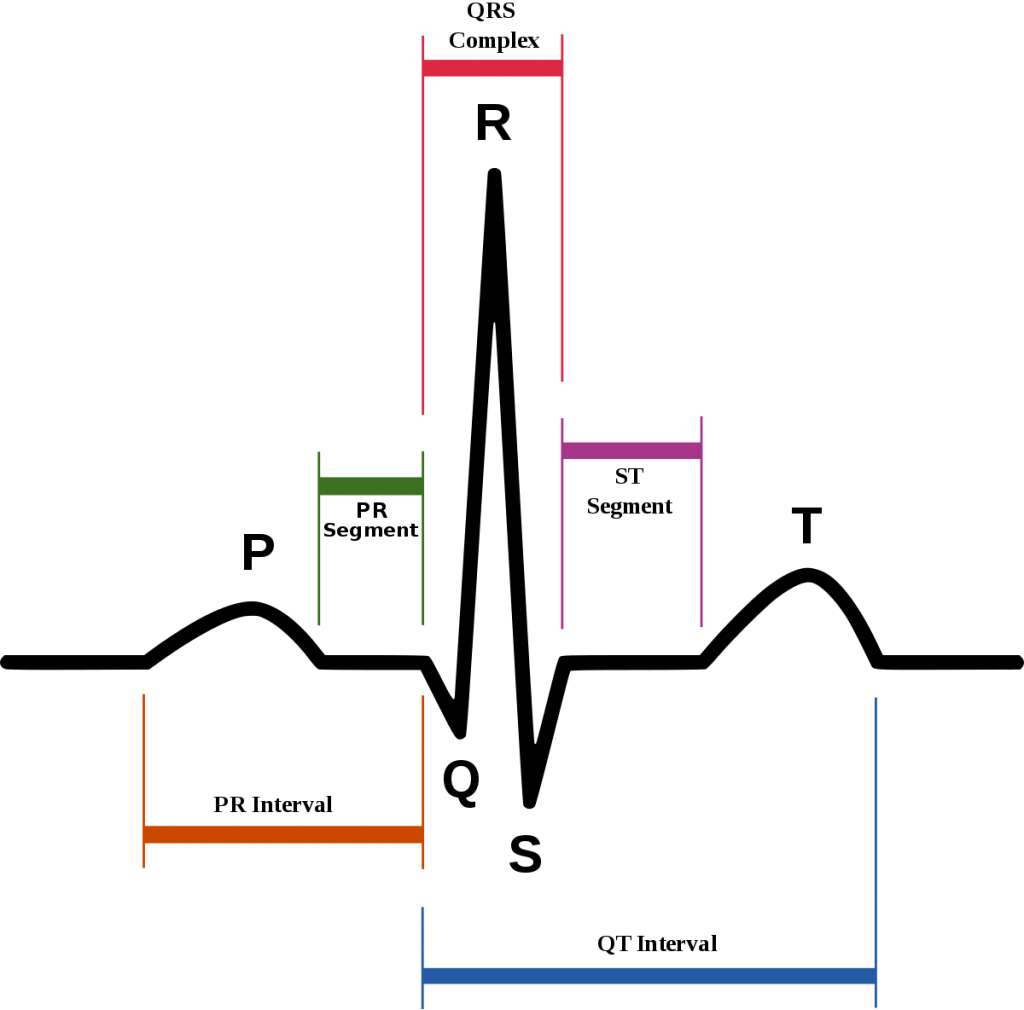
The teeth reflect different phases of the contraction of the heart. P reflects the moment of contraction and relaxation of the atria, R – excitation of the ventricles, T – relaxation of the ventricles. Special designations are also used for segments (gaps between adjacent teeth) and intervals (parts of the graph, including segments and teeth), for example, PQ, QRST.
Compliance of the stages of contraction of the heart and some elements of the cardiograms:
- P – atrial contraction;
- PQ – horizontal line, the transition of the discharge from the atria through the atrioventricular node to the ventricles. Q wave may be absent;
- QRS – ventricular complex, the most commonly used element in diagnosis;
- R – stimulation of the ventricles;
- S – myocardial relaxation;
- T – relaxation of the ventricles;
- ST – horizontal line, myocardial recovery;
- U – may be absent. The causes of the appearance of the prong are not clearly understood, but the prong is valuable for the diagnosis of certain diseases.
The following are some abnormalities on the ECG and their possible explanations. This information, of course, does not negate the fact that it is more expedient to entrust the decoding to a professional cardiologist who knows better all the nuances of deviations from the norms and related pathologies.
Major abnormalities and diagnosis
| Description | Diagnosis |
| The distance between the teeth of R is unequal | atrial fibrillation, cardiac block, weak sinus, extrasystole |
| P tooth too high (over 5 mm), too wide (over 5 mm), consists of two halves | atrial thickening |
| P wave is absent in all leads except V1 | rhythm does not come from a sinus node |
| PQ interval is extended | atrioventricular block |
| QRS extension | ventricular hypertrophy, blockade of the bundle of the His bundle |
| There are no gaps between QRS | paroxysmal tachycardia, ventricular fibrillation |
| QRS as a flag | heart attack |
| Deep and Wide Q | heart attack |
| Wide R (more than 15 mm) in leads I, V5, V6 | left ventricular hypertrophy, blockade of the bundle of the His branch |
| Deep S in III, V1, V2 | left ventricular hypertrophy |
| S-T above or below the contour more than 2 mm | ischemia or heart attack |
| Tall, double-haired, spiky T | heart overload, ischemia |
| T merging with R | acute heart attack |
Table of parameters of the cardiogram of an adult
| Metric | Value, c |
| QRS | 0.06-0.1 |
| P | 0.07-0.11 |
| Q | 0.07-0.11 |
| T | 0.12-0.28 |
| PQ | 0.12-0.2 |
The norm of the duration of the elements of the cardiogram of a child
| Metric | Value, c |
| QRS | 0.06-0.1 |
| P | > 0.1 |
| PQ | 0.2 |
| QT | > 0.4 |
The rates shown in the table may also depend on age.
The rhythm of contractions
Violation of rhythmic contractions is called arrhythmia . Irregular rhythm in arrhythmias is measured in percent. The irregular rhythm is indicated by a deviation of the distance between similar teeth by more than 10%. Sinus arrhythmia, that is, arrhythmia, combined with sinus rhythm, may be a variant of the norm for adolescents and young people, but in most cases indicates the beginning of the pathological process.
A kind of arrhythmia is extrasystole. He said it in the case when there are extraordinary reductions. Single extrasystoles (no more than 200 per day with Holter monitoring) can be observed in healthy people. Frequent extrasystoles appearing on a cardiogram in quantities of several pieces may indicate ischemia, myocarditis, heart defects.
Heart Rate
This parameter is the most simple and straightforward. It determines the number of cuts per minute. The number of contractions may be higher than normal (tachycardia) or lower than normal (bradycardia). The rate of heart rate in adults can range from 60 to 80 beats. However, the norm in this case is a relative concept, therefore, bradycardia and tachycardia are not always always evidence of pathology. Bradycardia can occur during sleep or in trained people, and tachycardia can occur during stress, after exercise, or at elevated temperature.
Norms of heart rate for children of different ages
| Age | HR, beats / min |
| Newborns | 140-160 |
| 6 months | 130-135 |
| 1 year | 120-125 |
| 2 years | 110-115 |
| 3 years | 105-110 |
| 5 years | 100-105 |
| 8 years | 90-100 |
| 10 years | 80-85 |
| 12 years and older | 70-75 |

Heart Rate Types
There are several types of heart rhythm, depending on where the nerve impulse begins to spread, leading to a contraction of the heart:
- Sinus,
- Atrial,
- Atrioventricular,
- Ventricular.
Normally, the rhythm is always sinus. At the same time, the sinus rhythm can be combined with both the HR and the normal heart rate, and the HR is below the normal. All other types of rhythms are evidence of problems with the heart muscle.
Atrial rhythm
Atrial rhythm also often appears on the cardiogram. Is the atrial rhythm normal or is it a type of pathology? In most cases, the atrial rhythm on the ECG is not normal. However, this is a relatively mild degree of heart rhythm disorder. It occurs in case of depression or malfunction of the sinus node. Possible causes – ischemia, hypertension, sick sinus syndrome, endocrine disorders. However, individual episodes of atrial contractions can also be observed in healthy people. This type of rhythm can take on both the character of bradycardia and the character of tachycardia.
Atrioventricular rhythm
The rhythm emanating from the atrioventricular node. With an atrioventricular rhythm, the pulse rate usually drops to less than 60 beats per minute. Causes – weakness of the sinus node, atrioventricular block, taking certain drugs. Atrioventricular rhythm, combined with tachycardia, can occur during heart surgery, rheumatism, heart attack.
Ventricular rhythm
With ventricular rhythm, contractile impulses spread from the ventricles. The frequency of contractions falls to a value below 40 beats per minute. The most severe form of rhythm disturbance. Occurs in acute myocardial infarction, heart defects, cardiosclerosis, heart failure, in the pre-diagonal state.
The electrical axis of the heart
Another important parameter is the electrical axis of the heart. It is measured in degrees and reflects the direction of propagation of electrical impulses. Normally, it should be slightly inclined to the vertical and be 30-69º. At an angle of 0-30º, it is said that the axis is horizontal, and at an angle of 70-90º, it is vertical. Deviation of the axis in one direction or another may indicate a disease, for example, hypertension or intracardiac blockades.
What do the findings on cardiograms mean?
Consider some terms that ECG decoding may contain. They do not always indicate serious pathologies, but in any case they require consulting a doctor for advice and sometimes additional examinations.
Atrioventricular block
Reflected in the graph as an increase in the length of the P-Q interval. Grade 1 disease is reflected as a simple lengthening of the interval. Grade 2 is accompanied by a deviation of the parameters of QRS (loss of this complex). At grade 3, there is no connection between P and the ventricular complex, which means that the ventricles and atria each work at their own pace. The syndrome in stages 1 and 2 is not life-threatening, but it requires treatment, as it can turn into an extremely dangerous stage 3, at which the risk of cardiac arrest is high.
Ectopic rhythm
Any heart rate not related to sinus rhythm. May indicate the presence of blockades, coronary heart disease, or be a variant of the norm. It may also appear as a result of glycoside overdose, neurocirculatory dystonia, hypertension.
Sinus bradycardia or tachycardia
Sinus rhythm on an ECG whose frequency is lower (bradycardia) or higher (tachycardia) than normal. It can be both a variant of the norm, and be a symptom of certain pathologies. However, in the latter case, this symptom most likely will not be the only one indicated in the transcript of the cardiogram.
Non-specific ST-T changes
What is it? This entry suggests that the reasons for the change in the interval are unclear, and more research is needed. It may indicate a violation of metabolic processes in the body, such as a change in the balance of potassium, magnesium, sodium ions, or endocrine disorders.
Disorders related to conduction inside the ventricles
As a rule, they are associated with conduction disturbances inside the nerve bundle of His. May affect the trunk of the beam or its legs. May result in a delayed contraction of one of the ventricles. Direct therapy for blocking His bundle is not performed, only the disease that causes them is treated.
Incomplete blockade of the right bundle of his bundle (NBPNPG)
A common ventricular conduction disorder. In most cases, however, it does not lead to the development of pathologies and is not their consequence. If the patient has no problems with the cardiovascular system, then this symptom does not require treatment.
Complete blockade of the right bundle of His (PBNPG)
This violation is more serious than an incomplete blockade. May indicate myocardial damage. Usually occurs in older and older people, rarely found in children and adolescents. Possible symptoms are shortness of breath, dizziness, general weakness and fatigue.
Blockade of the anterior branch of the left bundle of His (BPVLNPG)
Occurs in hypertensive patients who have had a heart attack. May also indicate cardiomyopathy, cardiosclerosis, atrial septal defect, mitral valve insufficiency. It has no characteristic symptoms. It is observed mainly in older people (over 55 years).
Blockade of the posterior branch of the left bundle of His (B3VLNPG)
As a separate symptom is rare, usually combined with blockade of the right bundle of the beam. May indicate a heart attack, cardiosclerosis, cardiomyopathy, calcification of the conduction system. The blockade is indicated by a deviation in the electrical axis of the heart to the right.
Metabolic changes
Reflect the malnutrition of the heart muscle. First of all, it concerns the balance of potassium, magnesium, sodium and calcium. The syndrome is not an independent disease, but indicates other pathologies. It can occur with ischemia, cardiomyopathy, hypertension, rheumatism, cardiosclerosis.
Low ECG Voltage
Electrodes mounted on the patient’s body pick up currents of a certain voltage. If the voltage parameters are below the norm, then they say about low voltage. This indicates a lack of external electrical activity of the heart and may be due to pericarditis or a number of other diseases.
Paroxysmal tachycardia
A rare condition that differs from normal (sinus) tachycardia, primarily due to the fact that it has a very high heart rate – more than 130 beats / sec. In addition, paroxysmal tachycardia is based on the improper circulation of an electrical impulse in the heart.
Atrial fibrillation
Atrial fibrillation is based on atrial fibrillation or flutter. Arrhythmia caused by atrial fibrillation can also occur in the absence of heart disease, for example, in diabetes, intoxication, as well as in tobacco smoking. Atrial flutter may be characteristic of cardiosclerosis, certain types of coronary disease, myocardial inflammation.
Sinoatrial blockade
Difficulty in the output of a pulse from a sinus (sinus) node. This syndrome is a type of sick sinus syndrome. It is rare, mainly in the elderly. Possible causes are rheumatism, cardiosclerosis, calcification, severe hypertension. It can lead to severe bradycardia, fainting, convulsions, breathing problems.
Hypertrophic myocardial conditions
Indicate overload of certain departments of the heart. The body feels this situation and responds to it by thickening the muscle walls of the corresponding section. In some cases, the causes of the condition may be hereditary.
Myocardial Hypertrophy
General myocardial hypertrophy is a protective reaction indicating excessive stress on the heart. May cause arrhythmias or heart failure. Sometimes it is the result of a heart attack. A type of disease is hypertrophic cardiomyopathy, a hereditary disease that leads to an incorrect arrangement of the heart fibers and carries the risk of sudden cardiac arrest.
Left ventricular hypertrophy
The most common symptom that does not always indicate severe heart disease. It may be characteristic of arterial hypertension, obesity, some heart defects. Sometimes observed and trained people, people engaged in heavy physical labor.
Right ventricular hypertrophy
A rarer, but at the same time, much more dangerous symptom than left ventricular hypertrophy. Indicates pulmonary circulation insufficiency, severe pulmonary diseases, valvular defects, or severe heart defects (Fallot’s tetrad, ventricular septal defect).
Left atrial hypertrophy
Reflected as a change in the P wave on the cardiogram. With this symptom, the prong has a double top. It indicates mitral or aortic stenosis, hypertension, myocarditis, cardiomyopathy. It leads to chest pain, shortness of breath, increased fatigue, arrhythmias, fainting.
Right atrial hypertrophy
Occurs less frequently than left atrial hypertrophy. There may be many causes – pulmonary pathology, chronic bronchitis, arterial emboli, tricuspid valve defects. Sometimes observed during pregnancy. It can lead to circulatory disorders, edema, shortness of breath.
Normocardia
Under normocardia or normisystole means normal heart rate. However, the presence of normysystolism does not in itself indicate that the ECG is normal and the heart is fine, as it may not exclude other pathologies, such as arrhythmias, conduction disturbances, etc.
Nonspecific T-wave changes
This characteristic is typical for about 1% of people. Such a conclusion is made in the event that it is not possible to unambiguously associate it with any other disease. Thus, for non-specific changes of the T wave, additional studies are needed. The symptom can be characteristic of hypertension, ischemia, anemia and some other diseases, and can also occur in healthy people.
Tachysystole
Also often called tachycardia. This is the general name for a number of syndromes in which there is an increased frequency of contractions of various parts of the heart. There are ventricular, atrial, supraventricular tachysystoles. Such types of arrhythmias as paroxysmal tachycardia, atrial fibrillation and flutter also belong to tachysystoles. In most cases, tachysystoles are a dangerous symptom and require serious treatment.
ST Heart Depression
Depression of the ST segment is often found in high-frequency tachycardias. It often indicates a lack of oxygen supply to the heart muscle and may be characteristic of coronary atherosclerosis. At the same time, depression is also observed in healthy people.
Edge ECG
This conclusion often scares some patients who find it on their cardiograms and are prone to think that “borderline” means almost “death”. In fact, such a conclusion is never given by a doctor, but is generated by the program analyzing the parameters of the cardiogram on an automatic basis. Its meaning is that a number of parameters are outside the normal range, but it is impossible to conclude unambiguously that there is any pathology. Thus, the cardiogram is on the border between normal and pathological. Therefore, upon receipt of such a conclusion, consultation of a doctor is required, and perhaps everything is not so scary.
Pathological ECG
What is it? This is a cardiogram, which clearly revealed some serious deviations from the norm. These can be arrhythmias, conduction disorders, or cardiac muscle feeding. Pathological changes require immediate consultation with a cardiologist, who must indicate a treatment strategy.
Ischemic ECG changes
Ischemic disease is caused by impaired blood circulation in the coronary vessels of the heart and can lead to such serious consequences as myocardial infarction. Therefore, the identification of ischemic signs on the ECG is a very important task. Ischemia at an early stage can be diagnosed by changes in the T wave (lifting or lowering). At a later stage, changes in the ST segment are observed, and in the acute phase, changes in the Q wave.
Decoding ECG in children
In most cases, deciphering the cardiogram in children is simple. But the parameters of the norm and the nature of violations may differ compared with those in adults. So, children normally have a much more frequent heartbeat. In addition, the dimensions of the teeth, spacing and segments are somewhat different.