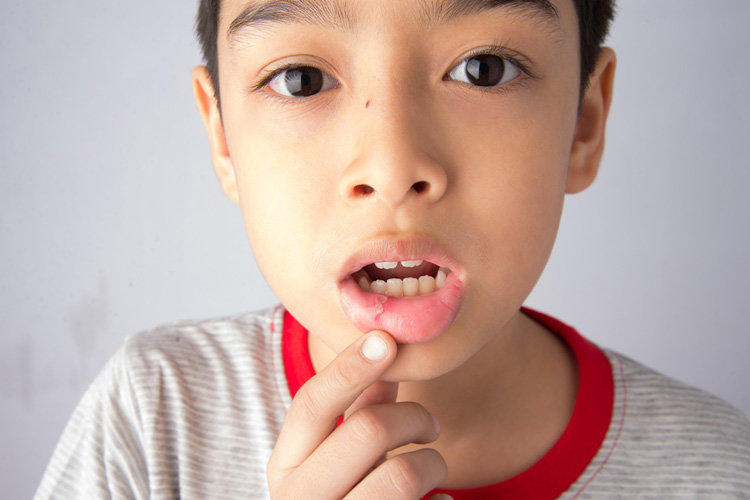
Stomatitis in children is a fairly common disease, defined as a heterogeneous group of diseases of various etiologies. At an early age, a child’s stomatitis can be caused both by infectious causes related to the imperfection of the immune system, and inflammatory processes provoked by injuries of the oral mucosa due to the desire to taste the surrounding objects “to taste”, to examine them with the lips and tongue. Stomatitis in children most often develops acutely, unlike adults, with concomitant intoxication of the body. Treatment of stomatitis in children depends primarily on the cause, the factor that caused the disease, and takes into account the characteristics of childhood.
- Children’s stomatitis: classification of the disease according to etiology
- Symptoms and treatment of fungal stomatitis in children
- Oral candidiasis: how to treat child stomatitis?
- Herpetic stomatitis in children: treatment and prevention
- Symptoms of herpetic stomatitis
- Therapy for herpetic stomatitis in children
- Causes and treatment of aphthous stomatitis in children
- How to treat stomatitis in a child, how to prevent aphthous stomatitis?
Children’s stomatitis: classification of the disease according to etiology
Childhood stomatitis has a certain periodization depending on the infectious agent and the cause of the disease. Of course, in any age period, all types of stomatitis may occur, but there are also regularities.
Fungal or candidal stomatitis develops in babies up to three years old, this is the so-called oral thrush. At the age from one to three years, herpetic stomatitis is noted with a high frequency with a decrease in specific immunity and infection, as well as the formation of Bernard aft in the sky.
The cause of aphthous stomatitis is injury to the mucous membrane of the palate during an unsatisfied sucking reflex, when the pacifiers are replaced with a finger, and can also develop due to prolonged contact with the nipple or pacifier of coarse rubber with a metal spoon. The injured mucous area is colonized by pathogenic microflora, contributing to the development of a long-term specific inflammatory process.
At school age, Bernard’s aphthous stomatitis often affects the inner side of the lower lip and can be triggered by allergic reactions, injuries when there is a pen, pencil, fingers in the mouth, decreased immunity, specific reactions to toothpaste or coarse food. Allergic types of stomatitis are also characteristic for this age period.
There are also mechanical (resulting from injury) stomatitis, not accompanied by bacterial inflammation, chemical type of stomatitis, resulting from burns of the mucous membrane under the aggressive influence of liquids (alkalis, acids, etc.) and physical stomatitis, which develops due to excessively hot, cold, spicy foods or drinks.
The increased incidence of mucosal stomatitis in children is due to several factors:
- the mucous surface of the mouth is so thin that it is easily injured;
- the reflex tendency to “pull in the mouth” and the sucking reflex both contribute to the colonization of the oral cavity by pathogenic agents, and frequent epithelial injuries – abrasions, scratches, burns;
- childhood immune system is not mature enough;
- The aseptic properties of salivary fluid inherent in adults are not developed due to the lack of specific enzymes.
All these causes lead to the development of inflammatory processes in the oral mucosa, and even stomatitis of mixed etiology, such as bacterial and fungal infections, can occur. Stomatitis in children can be acute or chronic, relapse, manifest in a mild inflammatory process, or affect the entire oral cavity, causing severe intoxication of the body. When stomatitis is detected in children, treatment is based on determining the cause of inflammation and the clinical picture of the disease.
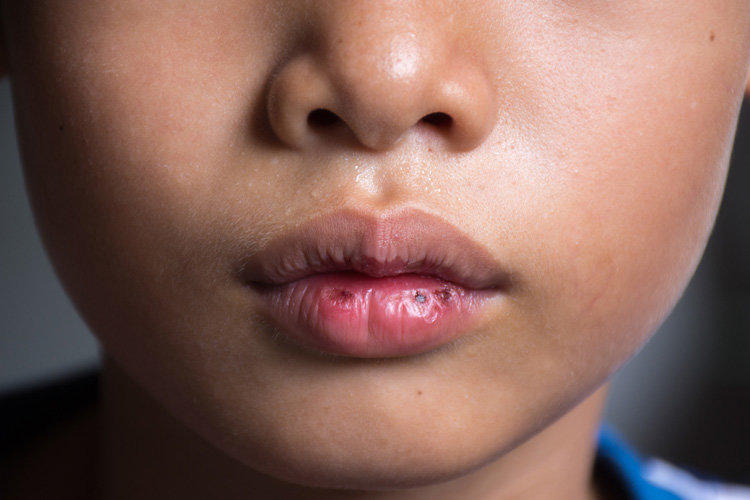
Symptoms and treatment of fungal stomatitis in children
Stomatitis in children caused by the fungus of the genus candida, otherwise called candidiasis of the mouth or thrush. It can develop during infection in the process of the infant passing through the birth canal of the mother, or it can occur as a result of the fungus infecting the mother’s nipples during breastfeeding and non-observance of hygiene rules. It is observed in premature babies, as well as after courses of antibiotic therapy, causing a decrease in specific immunity.
The symptoms and characteristic signs of fungal etiology stomatitis include:
- with rare exceptions – the absence of fever in the child;
- the presence of white, grayish cheesy plaque on the oral mucosa;
- easy removal of plaque does not cause concern, there is a hyperemia (redness) on the affected areas under patina, slight mucous bleeding is possible;
- lymph nodes are of normal size, not painful to palpation;
- primary localization of inflammation is focal, with subsequent damage to the entire mucosa;
- Candidosis delivers significant discomfort to the child: burning, itching, dryness, which is accompanied by a decrease in appetite, anxiety, sleep disturbance.
Oral candidiasis: how to treat child stomatitis?
If diagnosed with uncomplicated candidal stomatitis in children, local treatment is prescribed. Systemic antifungal drugs (prescribing Diflucan, Clotrimazole, Fluconazole) are indicated for older children or for severe, prolonged forms of candidiasis that cannot be treated by local therapy.
The treatment is based on the change in the acid-base balance of the oral cavity and the treatment with anti-fungal and antiseptic preparations. Candida fungus prefers high acidity, and increasing the performance of alkaline environment in most cases successfully helps the body to cope with the infection at the initial stage.
The methods of local therapy include:
- treatment of the oral cavity with sodium carbonate solution (baking soda): rinsing, wiping with gauze soaked in solution (1 tablespoon per cup of boiled water) with a frequency of 3 to 6 times a day, after each meal;
- processing and rinsing with Blue’s solution, 2% boric acid, borax solution in glycerin;
- use of local antifungal agents – creams, ointments for the oral cavity (Clotrimazole, Pimafucin, Nystatin, Candide). The treatment is carried out in accordance with the doctor’s prescriptions: the drugs are potent, if not following the prescription or interrupting the course can cause both side effects and the formation of microorganism resistance to the active substance, which significantly complicates further treatment.
In a healthy child with a good immunity and the absence of concomitant factors for the development of candidiasis, treatment is limited to local remedies, most often enough treatment of the oral cavity with a solution of baking soda. In the presence of a fungal infection in a baby while breastfeeding, therapeutic or prophylactic anti-fungal treatment of the breast areola of the mother is necessary, otherwise reinfection of the child is possible when candidiasis spreads to the nipple area (or primary presence).
In addition to prescribing stomatitis drugs in children, supportive therapy is also recommended, aimed at increasing the body’s resistance: vitamins are prescribed, medicines can be used to increase local immunity (Imudon for resorption, etc.).
Treatment of oral candidiasis also includes a specific antifungal and anti-traumatic diet: eliminating rough, spicy, salty, hot and cold foods to reduce inflammation and injury to the oral mucosa, as well as sour foods (vegetables, fruits, berries, dishes), sweets and high carbohydrate foods and drinks, as they create a favorable environment for the growth of the fungus.
Herpetic stomatitis in children: treatment and prevention
Herpes sores in the presence of the human herpes virus in the body and a decrease in the overall immunity. The period of the greatest frequency of this disease – from 1 to 3 years – is due to the weakening of the immunity received from the mother. When meeting for the first time with a herpes infection, the children’s body can react with acute stomatitis, accompanied by high fever and signs of severe intoxication of the body.
Herpetic stomatitis must be differentiated during diagnosis from other manifestations of viral diseases characteristic of childhood and accompanied by damage to the oral mucosa ( measles , scarlet fever, chickenpox).

Symptoms of herpetic stomatitis
Herpetic stomatitis has a fairly vivid clinical picture with the following manifestations:
- the appearance of areas of hyperemia, alternating with the formation of bubbles with a transparent or whitish content, with a red edging. With the development of the disease vesicular formations can spread to the outer surface of the lips, nasolabial triangle, nasal passages, then the bubbles burst with ulceration of the mucous membrane;
- the appearance of vesicles coincides with the onset of a rise in body temperature to febrile indices, which are poorly affected by antipyretic drugs.
- increase in local lymph nodes (jaw, cervical group);
- general intoxication of the body, manifested in nausea, vomiting, headaches, sleep disorders, etc.;
- lack of appetite due to pain in the mouth.
Herpetic stomatitis, occurring in a mild form, is accompanied by a small number of rashes (up to 6-7), no signs of inflammation in the lymph nodes, hyperthermia in low-grade indicators (up to 38 ° C), with the use of antipyretic agents the body temperature drops.
Therapy for herpetic stomatitis in children
Despite the fairly familiar herpes virus, severe herpetic stomatitis may require hospitalization due to high intoxication of the body and the risk of systemic spread of herpes in the body. Mild and moderate forms of the disease, the symptoms of which are described above, do not require placement in a hospital. For therapy prescribed symptomatic, antiviral treatment and related activities:
- Primary oral surgery can be carried out with a 3% solution of hydrogen peroxide, furatsilina. In the future, it is recommended to use herbal teas in the absence of allergic reactions (chamomile, sage, ready-to-eat Evkar, Ingafitol);
- as an antiseptic, disinfectant, depending on the age of the child, Lugol’s solution, Miramistin, Chlorhexidine, Rotocan, etc. are used;
- since herpetic stomatitis causes significant pain, prescribe anesthetics, local anesthetics, often combined action (antiseptic + anesthetic): Hexoral, Stomatidin, Mundizal-gel, etc. When not available, self-mixing of solutions with Novocain (0 , 5% solution, 2 ml per 100 ml of water);
- drugs of specific antiherpetic action (Acyclovir, Zovirax in the form of ointments) and general antiviral drugs (Oskolinovaya ointment, Bonafton) are used;
- for acute, severe, frequent relapses, it is possible to use anti-herpes drugs of systemic action as prescribed by a doctor;
- To speed up tissue regeneration and healing mucosal ulceration, an oil solution of vitamin A, Shostakovsky balm, sea buckthorn seed oil, dog rose, propolis preparations, etc. are used.
In the course of therapy, a sparing diet limiting spicy, acidic foods, coarse foods, hot and cold dishes is necessary.
During the course of the disease, as a preventive measure for infecting the rest of the family members, the child must have his own dishes and hygiene products.
Lack of treatment, even mild forms and failure to comply with the prescription of the doctor is dangerous recurrence of the disease, both in the form of stomatitis, and in other forms, for example, herpes conjunctivitis.
Causes and treatment of aphthous stomatitis in children
Aphthous stomatitis is typical for children a year and older. According to studies, aphthous stomatitis in children and adults occurs with a frequency of up to 4 cases per 10 people. The exact etiology of the disease is unknown, but there are many factors contributing to the formation of aphthous oral ulcers.
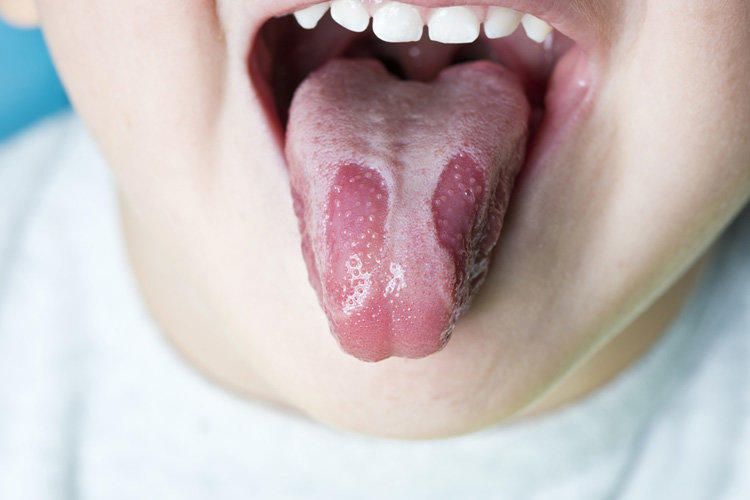
Ulcerative defects can be single and multiple, located on all parts of the oral mucosa. The so-called “geographical tongue” also refers to the aphthous type of stomatitis of allergic etiology.
What can cause the development of aphthous stomatitis? Allocate the role of injuries of the oral mucosa, food allergies and gluten, the role of hereditary susceptibility to aphthous ulcers, vitamin deficiencies, mineral deficiencies, factors of somatic diseases, in particular, diseases of the gastrointestinal tract and circulatory system, general immunodeficiency states.
How to treat stomatitis in a child, how to prevent aphthous stomatitis?
This form of stomatitis requires the identification of the cause of the disease and appropriate therapy. As a general direction of treatment, only local treatment with anti-inflammatory and antiseptic preparations can be distinguished, and the selection of the drug depends on the response of the patient. Perhaps the appointment of such solutions for the treatment of oral cavity, as Iodinol, Miramistin, Lugol solution, Hexoral, Rotocan, Shostakovsky balm, etc.
However, in addition to symptomatic treatment, it is necessary to identify the nature of the disease. Consultation often requires a dentist, allergist, gastroenterologist. Medicines are prescribed in accordance with the etiology, symptoms and stages of the disease and may include groups of antihistamine preparations for relieving allergy symptoms, remedies for treating diseases of the stomach, intestines, immunotherapy and vitamin therapy, oral hygiene at the dentist and hygienist, etc.
Physical procedures can also be included in the treatment methods, it is possible to prescribe electro- and phonophoresis, laser therapy depending on the stage of the disease and the age of the child.
Prevention measures include the following:
- regular oral hygiene, rinsing, use of dental floss to reduce the likelihood of bacterial inflammation;
- Correction of power supply. Some products contribute to irritation of the oral mucosa. With frequent relapses, exclusion from the menu of products such as milk, cheese, tomatoes and tomato paste, sour berries, fruits, juices, chocolate and cocoa in any form is recommended. Reduce the number of spicy and salty foods, as well as coarse food: chips, crackers, crackers that can injure the surface of the oral mucosa;
- Selection of toothpaste that does not contain sodium lauryl sulfate helps to avoid excessive draining of the mucous.